Healthy acidity
The vagina is highly acidic. This low pH comes from the microbes that live in female genitalia. On the mucous membranes, those are primarily lactic acid bacteria (from the genus Lactobacillus). These bacteria produce lactic acid, just as they do when they turn milk into yoghurt. This causes a high level of acidity, which most pathogens can’t handle. The vaginal microbiota, therefore, plays an important role in a woman’s health.

The body has at most places a pH value of 7. This is neutral. An exception is in the acidic environment in the vagina, which has a pH between 4.0 and 4.5.
Bacterial vaginosis
Research into the vaginal microbiota began more than a 100 years ago. Using light microscopes and bacterial cultures, researchers discovered that vaginal microbiota is out of balance in up to 25% to 30% of women. This is called bacterial vaginosis. In these women, the microbial diversity in their vaginas is much higher than average. In many cases, the bacteria Gardnerella vaginalis dominates the vagina, instead of the normal Lactobacillus bacteria. As a result, the pH is much higher.
Bacterial vaginosis can have serious health consequences. Among other things, it causes vaginal discharge, and increases the risk of Pelvic Inflammatory Disease (PID), uterine infections (endometritis) and premature birth. In addition, women with this abnormal vaginal microbiota are more susceptible to HIV and other sexually transmitted infections (STIs).
Before, during and after birth
The vaginal microbiota also plays an important role in the onset and development of the microbiome of a baby. In the uterus, the baby already receives the first, small amounts of bacteria from the mother. Much larger amounts of microbes follow, like Lactobacillus bacteria, coming from the vagina during labour. These lactic acid bacteria enter the baby’s intestines, where they help to digest the first mother’s milk.
First contact
Immediately after the birth, the baby also takes in bacteria from the environment and from mother’s milk. Since a newborn baby makes very little stomach acid, bacteria can easily reach the digestive tract and colonise there. These first bacterial species lay the foundation for the intestinal microbiome, and therefore also have an effect on the development of the microbiome in the future.
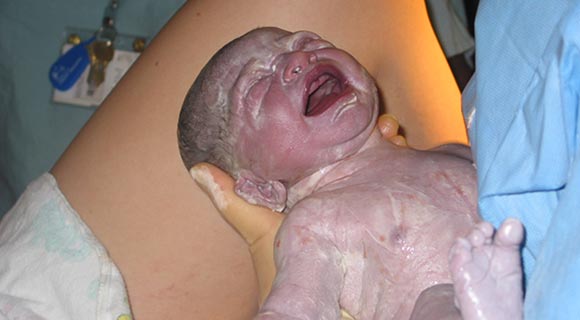
A baby receives a large amount of essential microbes from his mother at birth.
According to various studies, a Caesarean section can have a powerful influence on the development of the microbiome and the future health of a child. As a result, the child might obtain a less diverse microbial composition, which might not be able to fine tune the immune system, a possible cause for the correlation with an increased risk for autoimmune disorders later in life.
The male organ
The penis has a much lower number of microbes than the vagina. But, that hasn’t stood in the way of some pretty interesting discoveries in the past few years. Just like the vaginal microbiota, the microbiome of the penis is unique to every man. It is also dependant on age, sexual activity and whether or not he is circumcised. Researchers have proven that a circumcised penis has a clearly different microbial composition than an uncircumcised one. When the foreskin is removed, the number of anaerobic bacteria – the ones that can only live without oxygen – decreases significantly.

Foreskin of penis - 800 times magnified.
And microbes don’t just inhabit outer part of the male sex organ. The urogenital tract (the bladder, ureters, etc.), which was once considered to be sterile, also seems to have bacteria living in it.
