It is still unclear why this happens. At the University of Utah, they have now found some interesting clues in a study on platelets activity during a coronavirus infection.
Platelets, lifesavers
Platelets are the cells in our blood that prevent us from losing all of our blood if we accidentally cut our finger. They are the smallest cells in our blood and do not have a nucleus. They are formed in our bone marrow and are actually expulsions of the membrane of a mother cell. Because of this, they usually have a bit of a strange shape (see the yellow cell in the picture).
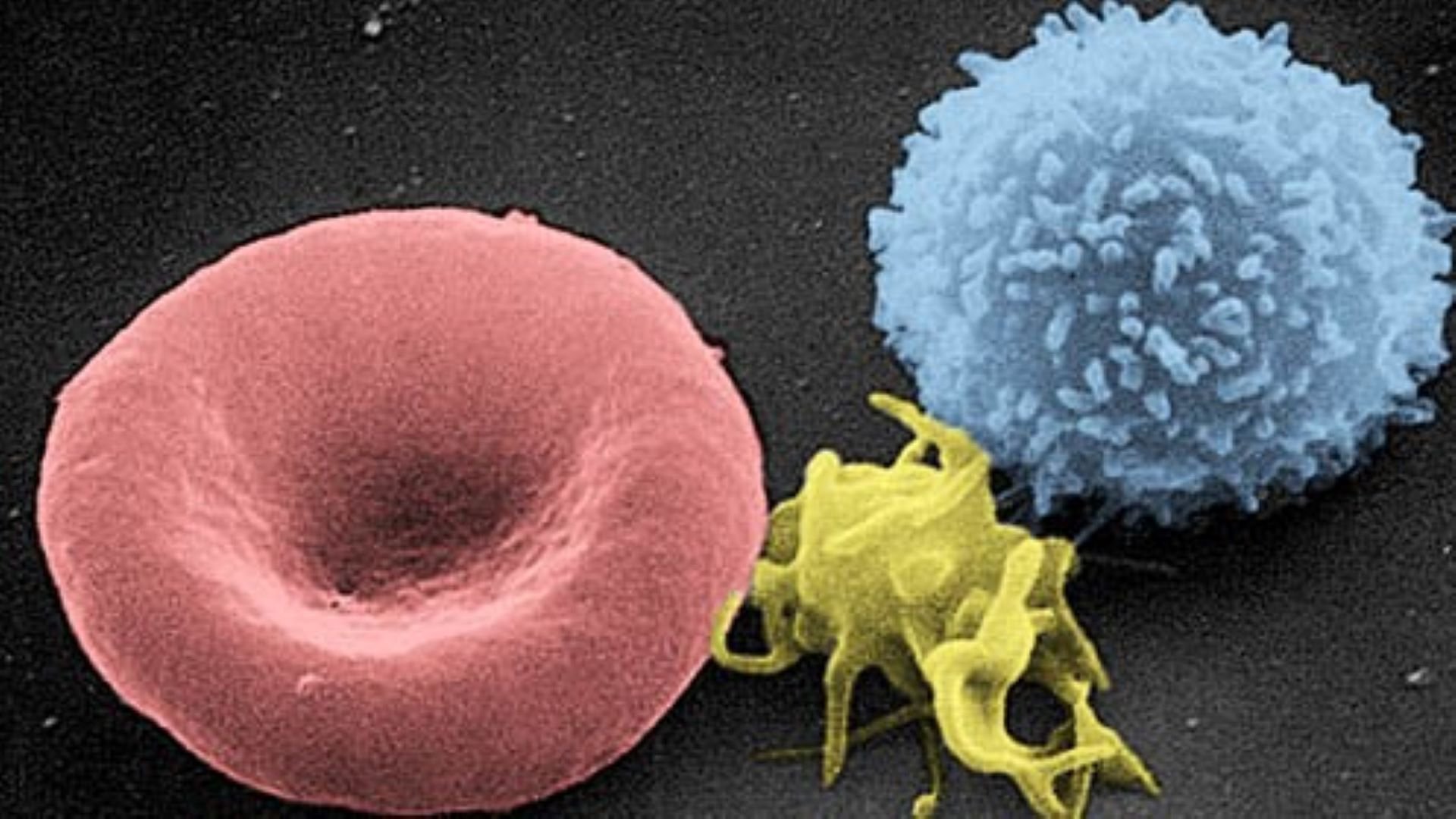
Colorized electron microscopy image of a red blood cell (red), platelet (yellow), and a white blood cell (blue).
This strange shape is also the strength of the humble platelet. If a blood vessel is ruptured anywhere, the platelet can register this and becomes "stickier". Subsequently, the sticky blood platelet attaches onto the damaged vessel wall through its hooks and bulges. Other platelets stick to these attached platelets, while the platelets all together also convert the protein fibrinogen into fibrin. Fibrin makes long wires and forms a kind of net (see the picture at the top of the article). The platelets and fibrin together form a tight barrier that stops blood cells from flowing out of the vessel, and your finger stops bleeding.
Blood clots
Unfortunately, platelets can also work against us. For example, in heart attacks or strokes where an important blood vessel is blocked. Usually this process starts with an accumulation of fatty substances somewhere in a blood vessel. This fat bulb can reduce the function of the blood vessel, but is even more dangerous if it releases and starts circulating through the blood. Platelets and fibrin in circulation can easily stick to this greasy ball. This creates a clot, which if it is large enough can clog a blood vessel in an important place, such as the brain or the heart. It turns out that corona patients have a considerably higher chance of forming these kinds of dangerous blood clots.
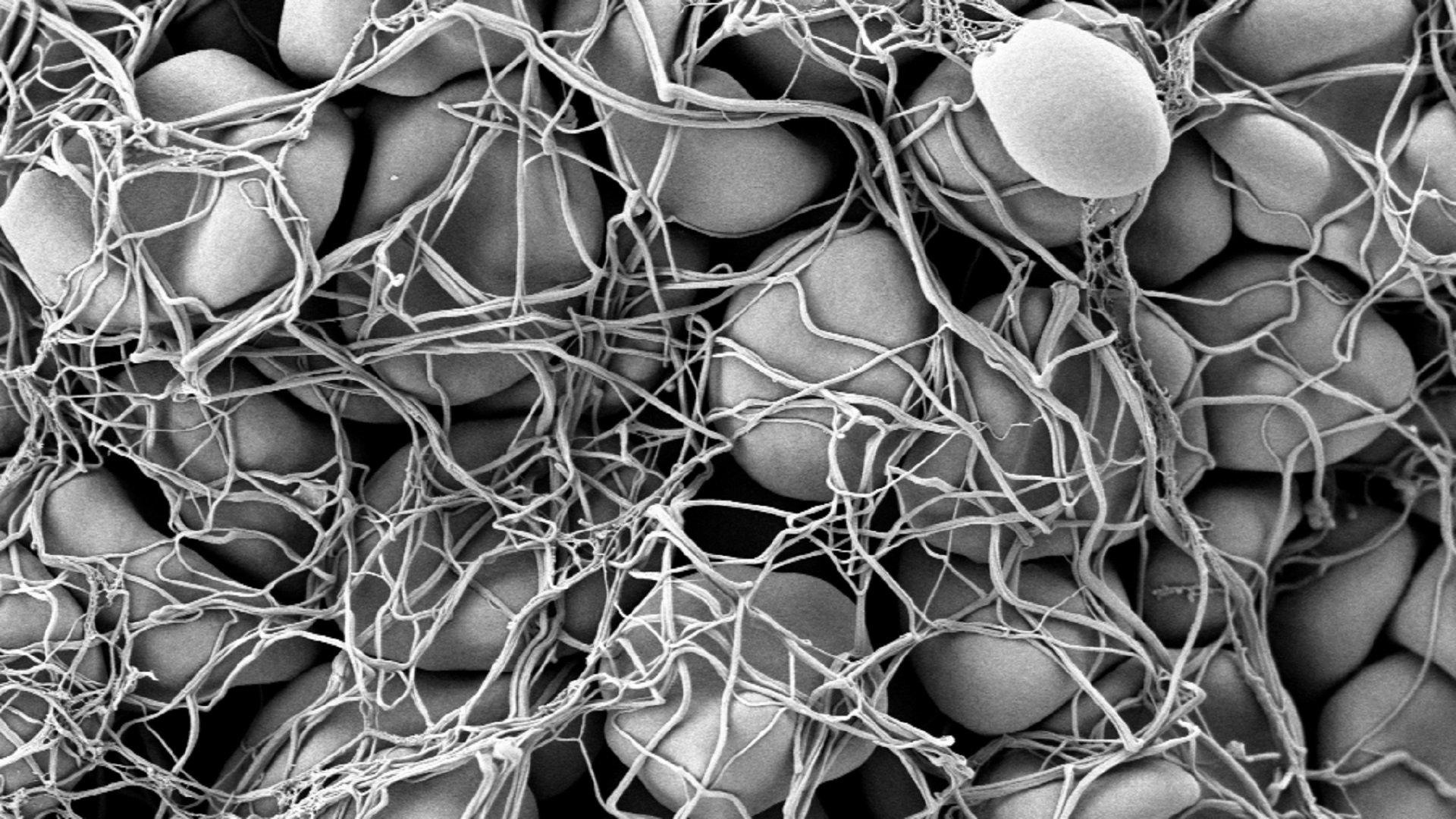
An electron microscopy image of a blood clot. The spheres are red and white blood cells, the net is made of platelets and the protein fibrin. (Wikimedia Commons; Fuzis)
Genetic changes
To find an explanation for the increased risk of blood clots, the blood of healthy subjects and corona patients was compared by mapping the DNA profile of their blood cells. When comparing the two profiles the researchers found that the DNA of the platelets in corona patients was different than in healthy subjects. These genetic changes lead to platelets becoming more active, and therefore stickier. This could significantly increase the likelihood of clots, and may explain why people with COVID can have serious complications such as stroke or heart attack. In addition, there are also indications that the hyperactive platelets boost the immune system, which is already very active due to the virus infection itself. This may for example aggravate strong inflammation in the lungs, which can lead to severe complications.
Like Mother like daughter?
How the coronavirus affects the DNA of the platelets is not yet fully understood. The researchers looked at whether the platelets themselves become infected with the virus, but this hardly seems to be the case. The theory now is that the source of the changes might be found in the platelet mother cells. When the genes of the mother cells are affected, they pass on the modified genes to all the daughter cells that they expel. The next step will be to find out whether the coronavirus does indeed make genetic modifications in the mother cells. The researchers hope that all these insights into the functioning of the platelets will lead to a better and faster treatment of complications in corona patients. For example, it can be examined whether existing medicines for blood thinning or suppression of certain branches of the immune system can effectively prevent or treat these complications.
| https://ashpublications.org/blood/article/doi/10.1182/blood.2020007214/461106/Platelet-Gene-Expression-and-Function-in-COVID-19 |
